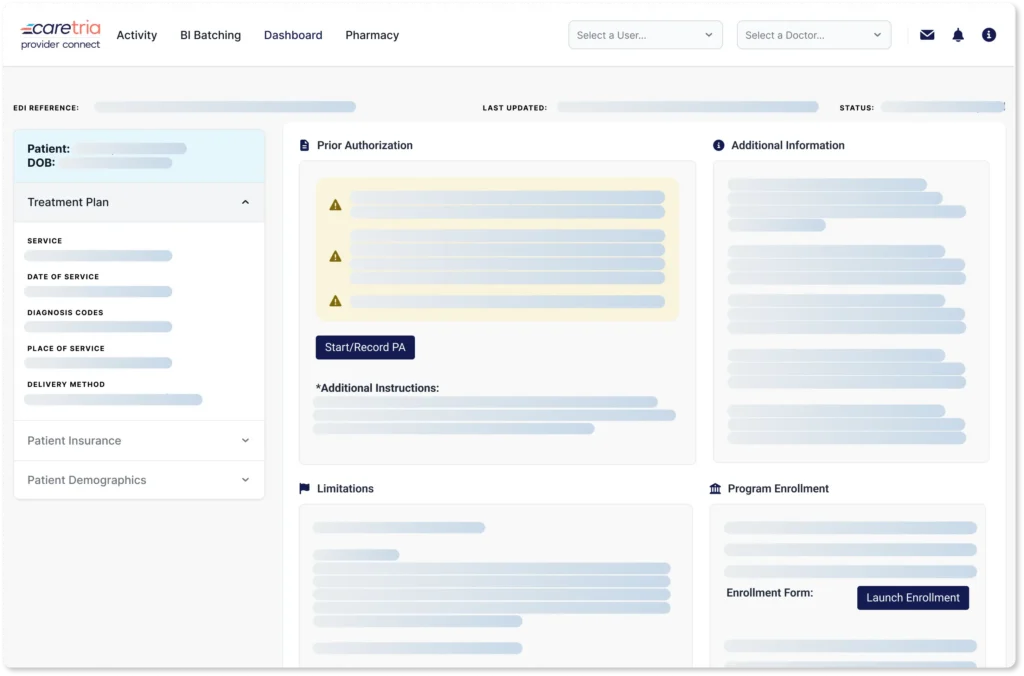
One platform, faster access
For over a decade, we have worked directly with specialty healthcare practices to provide the software solution they need to get patients to treatment faster. We’re changing the way patients get on – and stay on – treatment.

Tailored solutions for your role in patient care
Real-Time Benefit Investigation
Our application allows HCP’s the ability to submit requests and receive responses faster, resulting in quicker starts and stronger treatment adherence.
Electronic Prior Authorization
Achieve quicker approvals, reducing delays in patient treatment and improving overall efficiency.
Manufacturers Savings Program
Streamline patient enrollment tracking and connect patients to the savings programs they need to start and stay on treatment.
Payer Coverage
Share formulary information in real-time with providers during the treatment decision-making process.
Benefits
Provider Connect is no cost for healthcare practices
Medical & pharmacy benefits - in one platform
CareTria Provider Connect is the only software on the market that can verify benefits for specialty medications that fall under both medical and pharmacy benefits.
One portal for all patient access needs
Streamline your in-office workflow in a single platform with dedicated insights into the patient journey – from benefit investigation to prior authorization to co-pay enrollment.
Speed of return
Sponsored products full benefit investigations are returned instantly with the information the patient and the practice need to make informed treatment decisions. Prior authorizations yield an impressive return rate to eliminate any blockers to therapy.