Providers » Provider Solutions » Electronic Prior Authorization
Electronic prior authorization
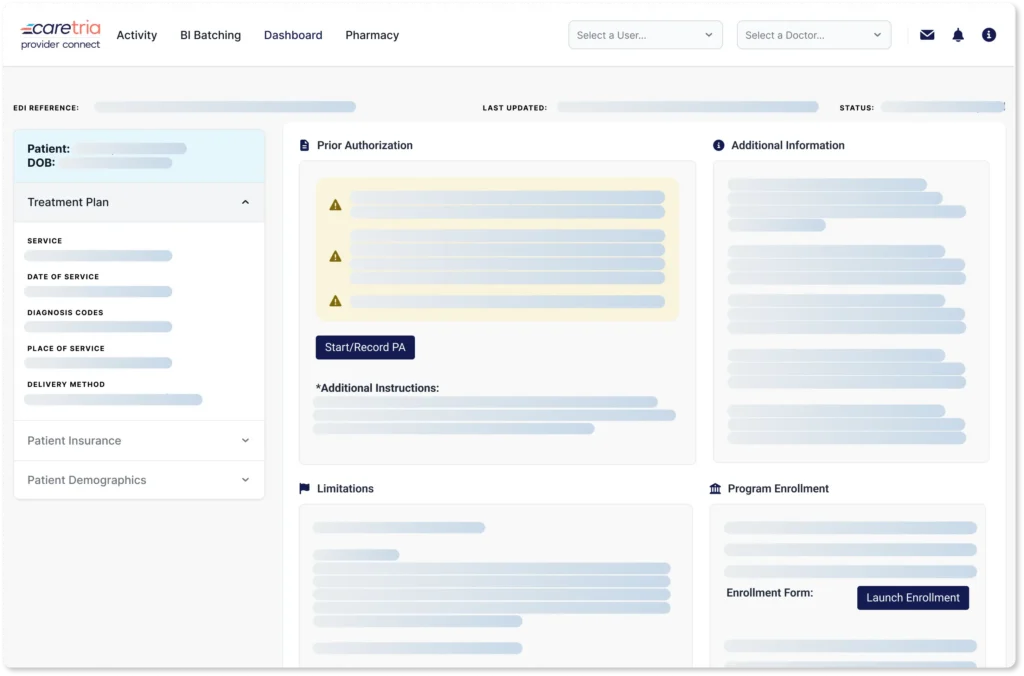
Finally, a user-friendly interface that simplifies the prior authorization process. With CareTria Provider Connect, you’ll achieve quicker approvals, reducing delays in patient treatment and improving overall efficiency.
About
e-Prior authorization in less than 3 days
Full benefit investigations return all of the information needed to make treatment decisions.
72hr
Average Payer Response Rate
94%
Provider Satisfaction
Benefits
Prior auth active monitoring for sponsored workflows
We understand the importance of tracking expiring prior authorizations. In an effort to achieve more streamlined processes centered around the prior authorization process and tracking of PA statuses, our software solution will notify you of any changes in a patient’s PA status. You’ll know exactly where your patient is in the process so there is no delay or pause in their life-changing treatments.
- Automation
- PA active monitoring
- Status of PA’s initiated by HCPs
- Status updates & notifications to HCPs