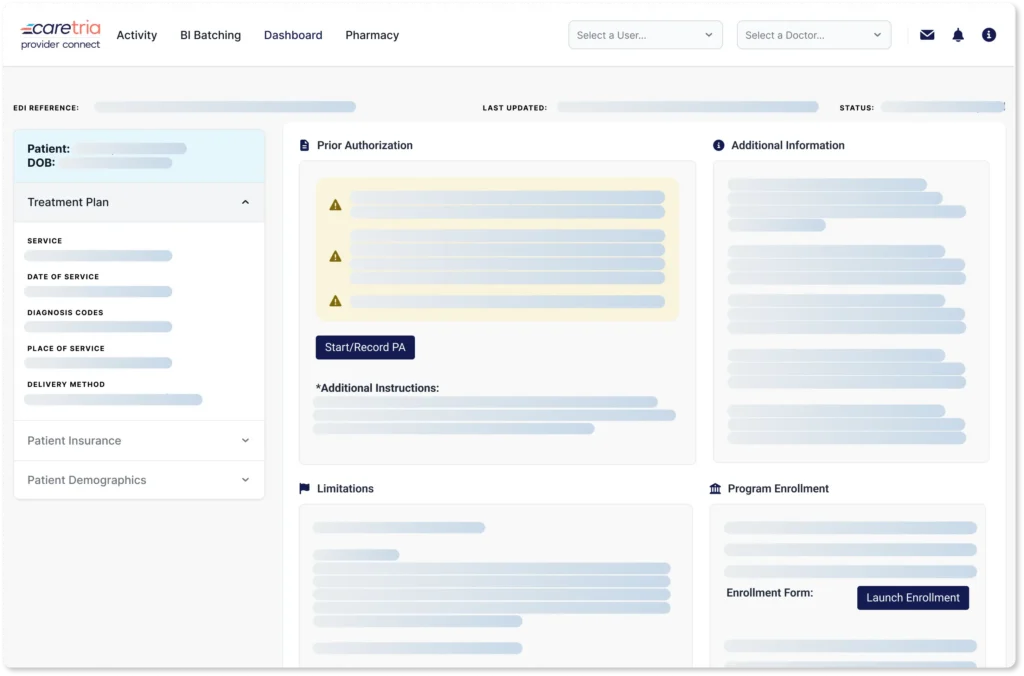
The fastest path from order to therapy starts here
CareTria’s Provider Connect accelerates patient access to specialty infusion and injection therapies by streamlining benefits verification, prior authorization, and manufacturer savings programs—all in one platform.
No cost for healthcare practices
CareTria’s Provider Connect is offered at no cost to practices, supporting access to real-time results without adding administrative expense.
Pharmacy and medical benefits in one easy-to-use platform
CareTria Provider Connect is the only platform on the market today to provide benefit investigations and prior authorizations for both medical and pharmacy benefits in one platform.
Coverage clarity instantly
With CareTria Provider Connect, you can turn benefit checks into immediate next steps and remove the guesswork from patient care.
Benefits
Provider Connect is no cost for healthcare practices
Medical & pharmacy benefits - in one platform
CareTria Provider Connect is the only software on the market that can verify benefits for specialty medications that fall under both medical and pharmacy benefits.
One portal for all patient access needs
Streamline your in-office workflow in a single platform with dedicated insights into the patient journey – from benefit investigation to prior authorization to co-pay enrollment.
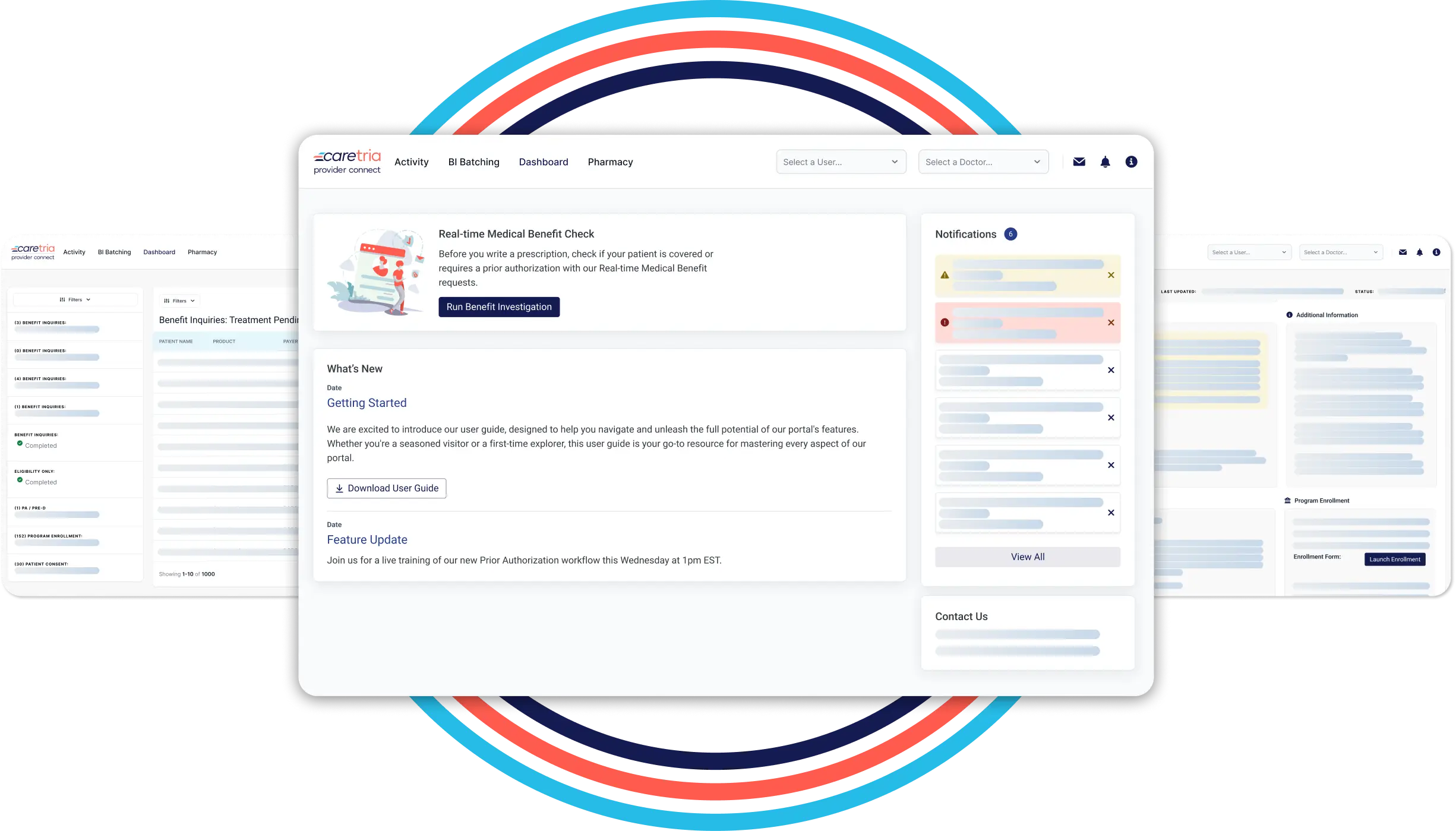
Speed of return
Sponsored products full benefit investigations are returned instantly with the information the patient and the practice need to make informed treatment decisions. Prior authorizations yield an impressive return rate to eliminate any blockers to therapy.
86%
Benefit Investigations Returned Instantly
95%
Prior Authorization Approval Rate
15K
Specialty Healthcare Providers

Created by specialty healthcare insiders to remove friction and fatigue from your day-to-day
Our unified portal supports over 1,400 payers and empowers healthcare practices, pharmaceutical manufacturers, and other partners to stay aligned.
The right tools for the entire treatment workflow
From real-time benefit investigations to electronic prior authorization and copay enrollment, CareTria Provider Connect powers the fastest path from order to therapy at the point of care.
01
Benefit Investigations
The authorization journey starts with the Benefit Investigation. Verify both medical and pharmacy benefits instantly with over 85% returning in 60 seconds or less.
02
Electronic Prior Authorization
Auto-populate prior auth forms, pre-validate fields, and track real-time status in one platform. No more faxing!
03
Manufacturer Savings Program
Enroll patients, manage EOB's, and track copay balances with less paperwork and faster fulfillment supporting stronger patient adherance.

Coverage in every therapeutic area
CareTria Provider Connect is purpose-built to support the clinical and administrative needs of high-cost, high-complexity treatments across a wide rage of healthcare specialities. Our platform is trust by practices nationwide in areas like:
Therapeutic areas served
- Rheumatology
- Gastroenterology
- Allergy & Asthma
- Neurology
- Rare Diseases
- Retina
- Orthopedics
- and more
This software has been an amazing tool that has benefitted our practice greatly.
The turnaround time for this was significantly quicker than going through other verification sources, and the information that we received was much more specific and reliable.
– Bill James, CFO, Talley Eye Institute
The platform is not only user-friendly but also remarkably efficient.
One of my favorite things about CareTria is their dedication to keeping their practice users informed with the latest updates. They go out of their way to ensure that we are informed about new insurance coverage/prior authorization requirements and new features on their platform. I wholeheartedly recommend CareTria Provider Connect to any practice user.
– Genesis Menendez, Benefits and Insurance Specialist, Sage Infusion
This is our "one-stop shop" for benefit investigations.
No more going to multiple sites with multiple logins and passwords. No wondering when the benefit investigationI will be returned or limitations on the number we can request. We upload our schedule weekly, sit back and receive our benefit investigations in a timely manner with special alerts for any issues. If we have any questions, a quick message sent within the portal gets a fast response.
– Chris Cagle, Tristate Arthritis